Misoprostol: women's autonomy in the tapestry of healthcare
Misoprostol is a synthetic prostaglandin medication used to prevent and treat stomach and duodenal ulcers, induce labor, cause an abortion, and treat postpartum bleeding due to poor contraction of the uterus.
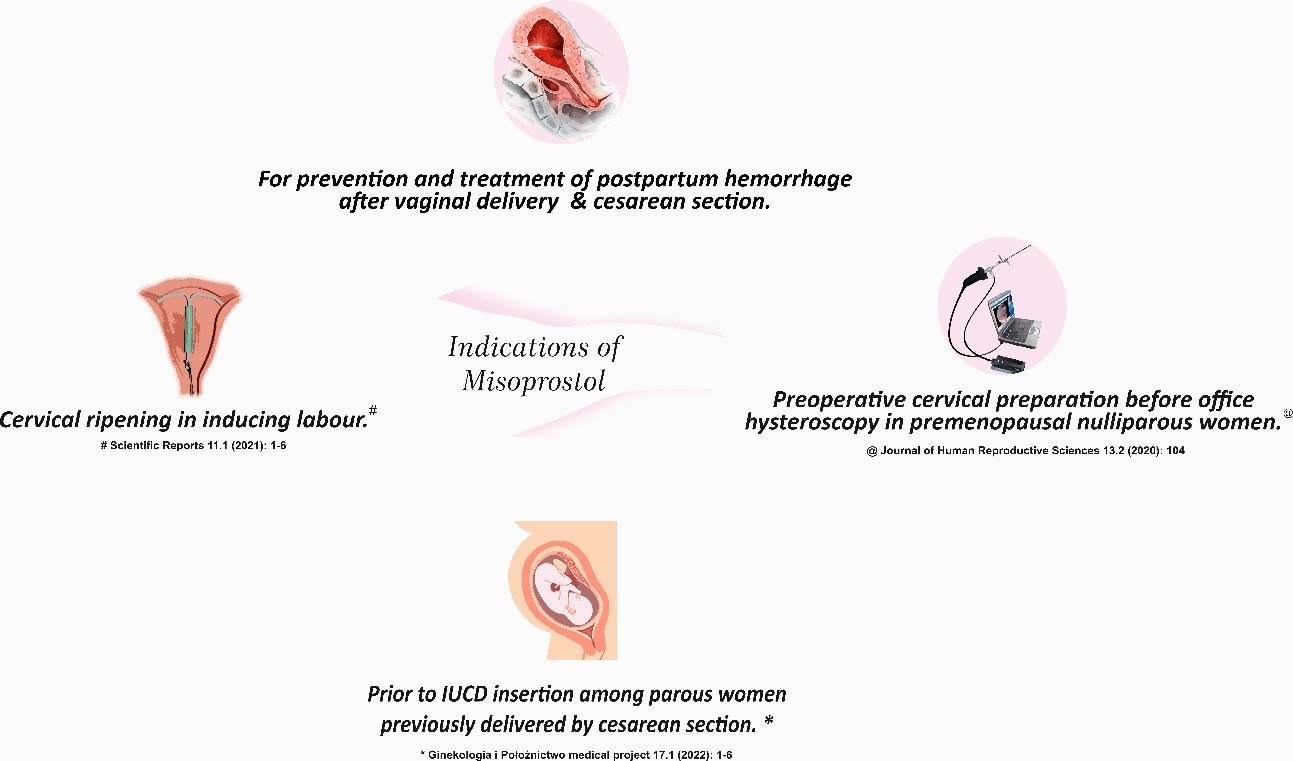
Misoprostol is commonly used in gynaecology for various purposes (fig. 1), including:
- Medical Abortion: Misoprostol is used in combination with another medication called mifepristone for medical abortion. It helps induce contractions of the uterus, leading to the termination of an early pregnancy. Medical abortion with misoprostol is generally considered safe and effective when conducted under proper medical supervision.
- Cervical Ripening: Misoprostol can be used to prepare the cervix for procedures such as dilation and curettage (D&C) or hysteroscopy. It helps soften and dilate the cervix, making these procedures easier and less uncomfortable.
- Labor Induction: In cases where labor needs to be induced, misoprostol may be used to promote uterine contractions and initiate labor. It can be an option when medical intervention is necessary for the well-being of the mother or baby.
- Management of Postpartum Hemorrhage: Misoprostol can be used to prevent and treat postpartum hemorrhage (excessive bleeding after childbirth). It helps contract the uterus and reduce the risk of excessive bleeding.
- Treatment of Missed Miscarriage: In some cases of missed miscarriage (when the embryo has stopped developing but the body has not expelled it), misoprostol can be used to help the body expel the non-viable pregnancy tissue.
- Induction of Fetal Demise: In cases where a pregnancy is non-viable and poses a risk to the mother’s health, misoprostol may be used to induce fetal demise before a medical procedure or induction of labor.
- Management of Menstrual Disorders: Misoprostol can also be used to treat certain menstrual disorders, such as heavy menstrual bleeding or irregular periods.
Misoprostol, like any medication, can have adverse effects. Some common adverse effects associated with the use of misoprostol include:
- Uterine Contractions and Bleeding: Misoprostol’s primary effect is to stimulate uterine contractions, which can lead to vaginal bleeding. This is expected during certain medical procedures like abortion or labor induction, but excessive bleeding can be a concern and should be monitored.
- Abdominal Pain: Uterine contractions caused by misoprostol can result in abdominal cramping and discomfort.
- Nausea and Vomiting: Some individuals may experience nausea and vomiting as a side effect of misoprostol.
- Diarrhea: Misoprostol can lead to diarrhea in some cases due to its effects on the smooth muscle of the gastrointestinal tract.
- Headache: Headaches are a possible side effect of misoprostol.
- Fever and Chills: Fever and chills can occur as a response to the uterine contractions induced by misoprostol.
- Dizziness or Light-headedness: Some people may feel dizzy or lightheaded after taking misoprostol.
- Allergic Reactions: While rare, allergic reactions to misoprostol are possible and could manifest as rash, itching, swelling, or difficulty breathing.
It’s important to note that the severity and occurrence of these adverse effects can vary from person to person. Additionally, misoprostol may have different effects depending on its specific use (e.g., medical abortion, cervical ripening, labor induction).
Misoprostol should only be used under the supervision of a qualified healthcare provider. They can provide guidance on its appropriate use, potential risks, and monitoring for adverse effects. If you experience any unexpected or severe adverse effects while using misoprostol, it’s important to seek medical attention promptly.
Misoprostol’s mechanism of action is primarily related to its effect on the smooth muscles of the uterus and the gastrointestinal tract. It is a synthetic prostaglandin E1 (PGE1) analog and exerts its effects through interaction with specific receptors in these tissues:
It’s important to note that misoprostol should only be used under medical supervision due to its potential side effects, contraindications, and interactions with other medications. Its use should be guided by a healthcare provider who can tailor the treatment to the specific medical condition and needs of the patient.
It’s important to emphasize that misoprostol should only be used under the guidance and supervision of a qualified healthcare professional. The dosage and administration of misoprostol can vary depending on the specific medical situation, and its use should be tailored to individual patient needs. Additionally, misoprostol can have side effects and potential complications, so its use should be well-informed and monitored by a healthcare provider.
Collagen: A structural scaffold
Collagen is the most abundant protein found in the human body and is a major component of various connective tissues. It is a fibrous protein that provides structural support, strength, and elasticity to different parts of the body, including the skin, bones, tendons, ligaments, cartilage, and blood vessels. It is essential for the structural integrity, strength, and resilience of bones. It serves as a scaffold for bone formation, provides attachment sites for bone cells, and plays a crucial role in bone remodeling and fracture repair. Adequate collagen production and maintenance are necessary for maintaining healthy bones.
Some key roles of collagen in bone are:
- Structural Support
- Bone Strength and Resilience
- Bone Formation and Remodeling
- Cell Attachment and Signaling
- Healing and Fracture Repair
There are several types of collagen, but the most common type is type I collagen, which accounts for about 90% of the collagen in the body. Other types include type II collagen found in cartilage, type III collagen found in blood vessels and skin, and type IV collagen found in the basement membrane of epithelial cells.
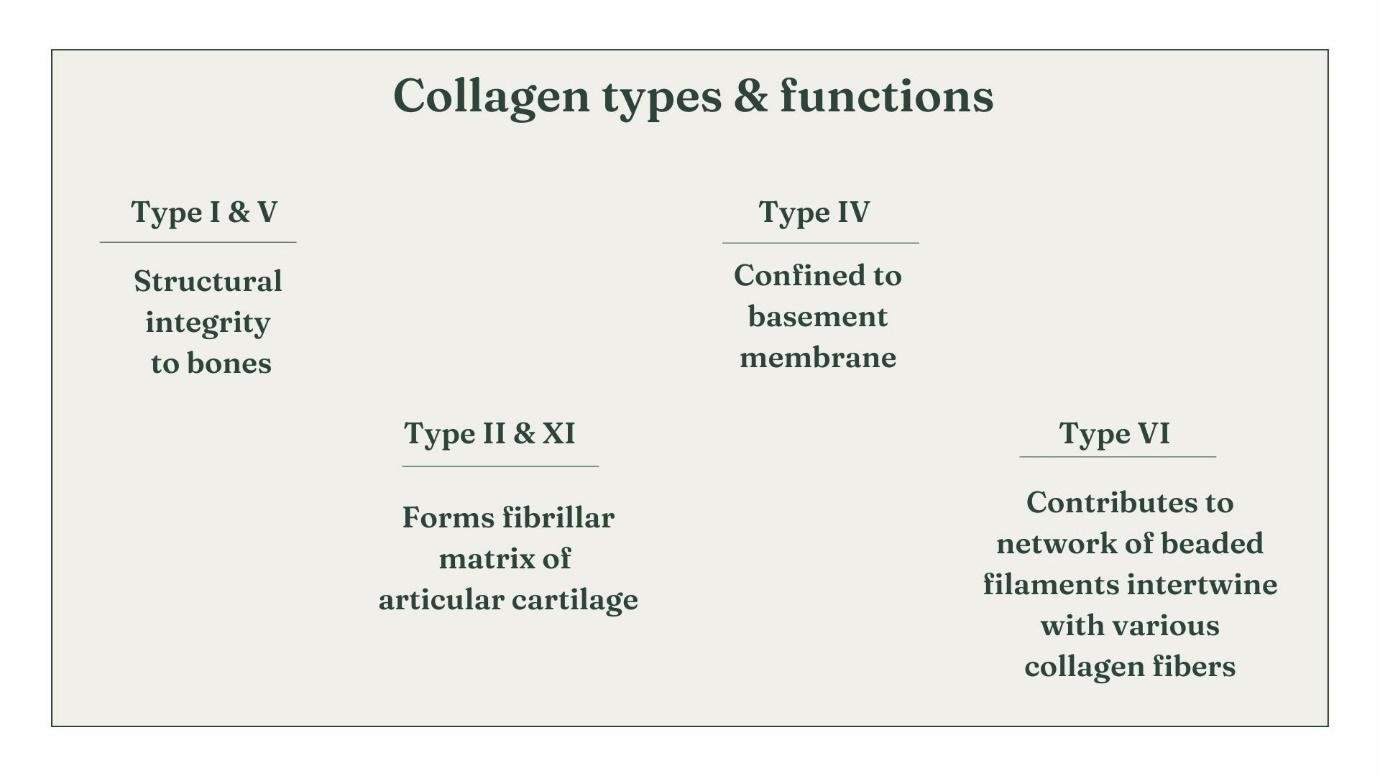
Type II collagen is a specific type of collagen that is primarily found in cartilage. It is a crucial component of the extracellular matrix in cartilage tissues and plays a significant role in maintaining the structure, function, and overall health of cartilage.
Cartilage is a flexible connective tissue that acts as a cushion between bones in joints, providing smooth movement and absorbing shock. Type II collagen makes up the majority of collagen in cartilage, accounting for approximately 50-60% of the total collagen content.
Some key features and functions of type II collagen are:
- Structure and Stability: Type II collagen fferoorms a unique triple helix structure, similar to other types of collagen. This structure provides strength, stability, and resistance to tensile forces, allowing cartilage to withstand pressure and maintain its shape.
- Support for Joint Health: Type II collagen is crucial for maintaining the health and integrity of joints. It helps to maintain the smooth and frictionless surface of cartilage, allowing bones to glide against each other smoothly during joint movement. Type II collagen also contributes to the structural integrity and shock-absorbing properties of cartilage, which are essential for joint function and preventing excessive wear and tear.
- Cartilage Regeneration: Type II collagen is involved in the process of cartilage regeneration and repair. During injury or damage to cartilage, cells called chondrocytes produce type II collagen to rebuild and restore the damaged tissue. Type II collagen provides a framework for the deposition of other components of the extracellular matrix, facilitating the regeneration and remodeling of cartilage.
- Immune Function: Type II collagen has been studied for its potential immune-modulating properties. It is believed to play a role in oral tolerance, which refers to the body’s ability to tolerate specific substances without triggering an immune response. Oral supplementation of type II collagen has been investigated for its potential benefits in autoimmune conditions affecting the joints, such as rheumatoid arthritis.
With age, the production and quality of collagen may decline, leading to various signs of aging, such as wrinkles, sagging skin, and joint stiffness. Consequently, collagen supplementation has become popular to support skin health, joint health, and overall well-being.
It’s important to note that collagen is obtained from various sources, including animal-derived sources like bovine or marine collagen, as well as plant-based sources like collagen synthesized through recombinant DNA technology. These supplements are typically marketed for joint health support and are commonly used by individuals with osteoarthritis or other joint-related conditions. These collagen sources may have different properties and benefits, and it’s advisable to choose collagen supplements based on individual preferences and needs. It is important to consult with a healthcare professional before starting any new supplements, especially if you have specific health concerns or if you’re taking other medications.
- Kisling, Andrew, Robert M. Lust, and Laxmansa C. Katwa. “What is the role of peptide fragments of collagen I and IV in health and disease?.” Life sciences228 (2019): 30-34.
- Gencoglu, Hasan, et al. “Undenatured type II collagen (UC-II) in joint health and disease: a review on the current knowledge of companion animals.” Animals10.4 (2020): 697.
Folic acid: why it is essential for hematopoiesis?
Folic acid, also known as folate or vitamin B9, is a water-soluble vitamin that plays a crucial role in several bodily functions. It is an essential nutrient required for the synthesis and repair of DNA, as well as for cell division and growth.
Folic acid is particularly important during periods of rapid cell division and growth, such as pregnancy and infancy. Adequate intake of folic acid is vital for the proper development of the fetal neural tube, which later becomes the baby’s brain and spinal cord. Pregnant women are often advised to take folic acid supplements to reduce the risk of certain birth defects, such as neural tube defects.
In addition to its role in prenatal health, folic acid is also involved in the production of red blood cells and in the metabolism of amino acids, which are the building blocks of proteins. It helps in the formation and maturation of red blood cells and assists in carrying oxygen throughout the body.
Foods that are rich in folic acid include leafy green vegetables (such as spinach and kale), legumes (such as lentils and chickpeas), citrus fruits, fortified cereals, and liver. However, it can be challenging to get enough folic acid through diet alone, especially for pregnant women, which is why supplements are often recommended.

Folic acid, or vitamin B9, plays a crucial role in hematopoiesis, which is the process of blood cell formation. Here’s how folic acid is involved in hematopoiesis.
- Red Blood Cell Formation: Folic acid is essential for the production and maturation of red blood cells, also known as erythrocytes. It is required for the synthesis of DNA and the proper division and development of red blood cell precursors in the bone marrow. Folic acid supports the production of healthy red blood cells, which are responsible for carrying oxygen to tissues and removing carbon dioxide.
- DNA Synthesis in Blood Cells: Folic acid is necessary for the synthesis and repair of DNA, which is critical for the development and maturation of all blood cells, including red blood cells, white blood cells, and platelets. DNA is the genetic material that provides instructions for cell growth, division, and specialization. Folic acid ensures that DNA is synthesized properly during the formation of blood cells.
- Prevention of Anemia: Anemia is a condition characterized by a decrease in the number of red blood cells or a decrease in their ability to carry oxygen effectively. Folic acid deficiency can lead to megaloblastic anemia, where red blood cells are larger than normal and immature due to impaired DNA synthesis. Adequate folic acid levels are necessary to prevent anemia and support the production of healthy red blood cells.
- Cell Division and Growth: Hematopoiesis involves the continuous division and differentiation of blood cell precursors to produce mature blood cells. Folic acid is required for cell division and growth, providing the necessary building blocks for DNA synthesis. Without sufficient folic acid, the process of hematopoiesis may be disrupted, leading to impaired blood cell production.
It’s important to note that folic acid works in synergy with other nutrients, such as vitamin B12 and vitamin B6, in the process of hematopoiesis. These vitamins are involved in the metabolism and utilization of folic acid, ensuring its proper function in blood cell formation. Adequate intake of folic acid and other B vitamins is essential for maintaining a healthy hematopoietic system.
It’s worth noting that folic acid is the synthetic form of the vitamin, commonly found in supplements and fortified foods. Folate, on the other hand, refers to the naturally occurring form of vitamin B9 found in foods. Both folic acid and folate are metabolized in the body to produce the active form, called 5-methyltetrahydrofolate (5-MTHF), which is responsible for the vitamin’s functions.
While folic acid is generally safe for most people when taken within recommended dosage levels, excessive intake through supplementation can mask vitamin B12 deficiency and may have adverse effects. It is always advisable to consult with a healthcare professional before starting any new dietary supplements, especially if you have specific health conditions or concerns.
1. Mikkelsen, Kathleen, and Vasso Apostolopoulos. “Vitamin B12, folic acid, and the immune system.” Nutrition and immunity (2019): 103-114.
